Warning: this post may just be an excuse for me to vent about all the uniquely Congolese, frustrating, odd, and wonderful things that have happened to me here!
“Only in the Congo.”
If you live in the Republic of Congo long enough, you will inevitably find yourself saying this in exasperation or in good humour, and sometimes both. My most recent utterance was that of exasperation, as I found out I would not be able to order a single lab test here for 4 days because it was the long weekend in spite of having 2 very ill patients!
The only explanation I have for this, is found in the Congolese word for tomorrow, lobe (pronounced low-bay or low-bee). This is a word they have for tomorrow, and yet I am told, it only means some time in the future! It could be a day, a few days, a week! Maybe this would be her response as to why we couldn’t get it done, we’ll do it lobe.
Their disconnect with time is not limited to the future. The past is often even murkier, which is a difficult thing when trying to ask someone about their medical history. Sometimes this gets to an extreme, like an Aka gentlemen who didn’t know how old he was! When I pressed the question, he got out an ID card issued by the government some years ago that had a generic birthday documented that would make him far too young. They explained they get these cards and he probably just told them he was born sometime in the 1970’s, so that’s what was documented!
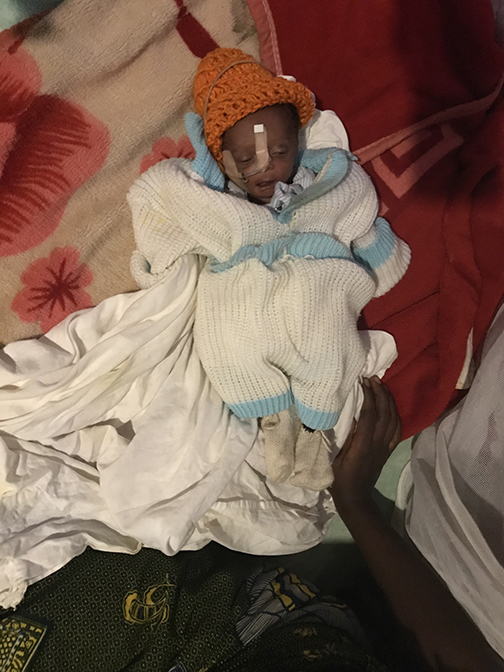
I had this happen again during rounds on the pediatric ward. I came to a young boy, and all that was on his chart for his age was a question mark. He was the most malnourished patient I have seen here, and was tall enough to be around 2 years old. I could see each and every rib, and he was lying in his own feces. It was heart wrenching. His current guardian was an elderly relative, who explained that his parents lived in Brazzaville but had shipped him up here and she was the only one to take him in!
A reason for a lot of the kids being malnourished is not a lack of food, most families can get enough for their kids from the jungle and their gardens. The problem is more often that they only feed the kids when they cry. So if you get a really content newborn baby, a mother may only be feeding them every 4-5 hours! There is a real lack of understanding of basic nutrition.
This isn’t the only misunderstanding. I work at a mission hospital, which pays a salary only to the local workers. I think many would understand this concept back home, but here people just can’t understand it. I realized this one day when we were talking about a patient having to pay their bills and I asked if they thought I was getting paid to be here. Everyone on the unit thought I was being paid well to work here!

It is very bizarre to come across these ideas, yet I get it. Why wouldn’t you distrust authority here? Medicine here is plagued with fraud. I have heard everything from the counterfeit medications at the pharmacies to a person performing bogus xrays out of his mud hut. This ruse turned out to be him flashing lights at the patient and then he would produce an xray film of the appropriate body part (most of the time) that he had stolen! Only in the Congo.
All these things really start to wear you down over time! It makes life for local people here incredibly complicated, unjust, and frustrating. So then, it makes a lot more sense when they approach life and work with an easygoing attitude. If you got frustrated every time you were slighted here, you would probably go mad!
There are also a lot of positive things that would happen only in the Congo. Like lounging after supper to the sound of distant drums that are so incredibly regular that it feels like the pulse of Africa. Or the singing that is done with the drums; it is so simple yet profoundly beautiful!
One of my favourite things is the ways they can say hello. In Lingala, you can say a simple “Mbote” for hello, or you often here “Mbote mingi!” This roughly translates to “hello very much”, or a respectful and exuberant hello! This would then be followed by shaking hands with their left hand clasped on their right forearm, a way of showing respect. Similarly, they will often wave with both hands and a slight bow to show respect. Steph and I are always greeted emphatically by kids as we ride through town on our bikes with hello’s, mbote’s and moondele (their word for white person)! If you forget it is only because you are white, it almost feels like you are a celebrity.
The Aka people (pygmy) are also one of my favourite things you will only find here! They are so friendly but have gone through so much abuse at the hands of people (the Bantu) who treat them as sub-human. They took us on a jungle walk and showed us their medicinal plans, got a vine for us to swing on, built a shelter and fed us their edible fruits, including cocoa!

Lastly, the close community is palpable here. People often pay their hospital bills with their own type of insurance system. People ask others in their family and community for help and raise money for one another on an as needed basis! They are very caring and helpful in this way, and always willing to humour me with a conversation in broken French. Even with complete strangers, people will stop and chat for some time!
Only in the Congo could I find things so incredibly frustrating and beautiful at the same time!